Interventions for Preterm Birth: an overview of Cochrane Systematic Reviews
Posted on 19th December 2018 by Lucy Beresford
Whats the problem?
Across the world, over 34% of infant deaths can be attributed to preterm birth (PTB) (Callaghan et al, 2006). Whilst advances in neonatal medicine are improving these mortality rates, the lost weeks of fetal development increase the risk of morbidities. These are likely to have significant, long-lasting impacts on a child, their family and the economy. An abundance of research has evaluated a variety of interventions aimed at preventing preterm birth. However, conflicting evidence makes it difficult to decipher what is actually beneficial.
A recent overview of Cochrane systematic reviews summarises some of the interventions used to reduce the risk of PTB. This will help clinicians and other stakeholders make evidence-based decisions with the aim to improve the impact of premature delivery.
You can learn more about how Cochrane overviews of reviews differ from a systematic review here.
What worked?
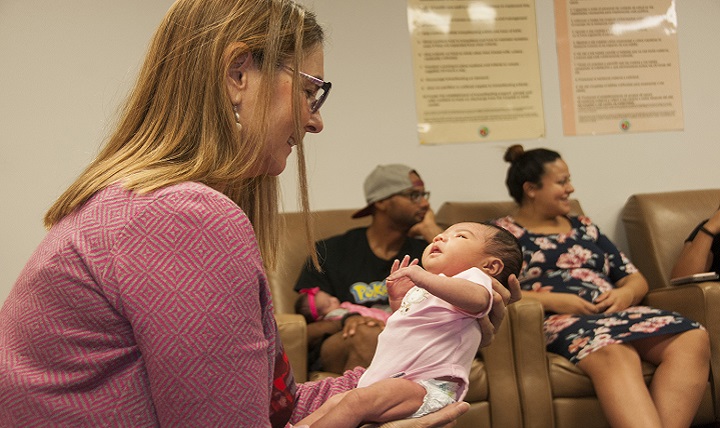
36 systematic reviews evaluated interventions for preventing premature delivery. Cervical cerclage (cervical stitch) showed clear benefit for women at high risk of PTB, but different interventions benefited those at a lower risk. These included zinc supplements and antenatal infection screening. However, midwife-led continuity care (MLCC) was the most effective intervention, reducing both PTB rates and infant mortality.
The findings provide promising results regarding the effectiveness of some interventions. However, many of these targeted specific populations of women. Consequently, the effects may be not be the same for the general population. For example, zinc tablets were beneficial for women with poor nutrition, but the effect may not be as significant for those who eat a balanced diet.
Many interventions were found to have an unknown harm or benefit at reducing premature delivery or neonatal mortality. For low-risk women, alternative antenatal care, calcium and vitamin supplements, routine ultrasounds and thyroid screening were shown to have clear evidence of no effect of equivalence, as was the case for bedrest and preventative prescriptions of antibiotics for high-risk mothers.
How good was the evidence?
There was a lack of high-quality evidence for effectiveness of interventions in women with multiple pregnancies. 40% of twins are born prematurely, so the need to find effective treatments to reduce the risk in these women is of high priority (Goldenberg et al, 2008).
Medley et al (2018) did not evaluate some of the most commonly used interventions in preventing PTB (e.g cervical length screening and progesterone supplementation). This was due to lack of current evidence. However, Medley et al (2018) point out that there are ongoing reviews evaluating the effectiveness of these interventions. This research could then be utilised when deciding on the most appropriate intervention for an expectant mother.
What does this change?
Midwife-led continuity care was the most effective intervention for reducing the risk of PTB and perinatal mortality. This promotes the use of one midwife throughout a woman’s pregnancy, childbirth and post-natal period (Sandall et al, 2016). The reasons for why the MLCC is effective is likely to be complex, but its benefits in reducing fetal mortality and PTB, as well as other adverse maternal outcomes, are notable. Research needs to be conducted to assess MLCC’s benefits for women at high-risk of PTB, as they are likely to be in need of a more complex care plan.
Many interventions given as a cautionary measure to women at low risk of premature delivery were not effective at reducing the risk of preterm birth. With limited resources available for the NHS, initial screening would provide valuable stratification of those of high risk. These women could then go on to receive the more resource-intense interventions with the aim of reducing their risk of PTB.
This summary presented clear evidence regarding the ineffectiveness of a variety of interventions. It could be argued that the administration of these interventions should be cautioned against.
What can we conclude?
In conclusion, Medley et al (2018) summarise the latest evidence regarding the effectiveness of a variety of preterm birth interventions. Midwife-led Continuity Care was the most effective at reducing the risk of premature birth and perinatal mortality. Whilst this may be resource intensive, the beneficial long-term effects on not only PTB and infant mortality but to overall infant and parental health may help to reduce costs in the future.
An important priority for research is updating systematic reviews on interventions not covered in this overview. This would provide a more comprehensive evaluation of the possible interventions, allowing stakeholders to make informed decisions when implementing the research into policy and practice.
Finally, this study signals the importance of individual differences in expectant mothers. Therefore, it is important to gain an insight into the woman and her history before deciding on the most suitable plans for her pregnancy.
It should also be noted that not every woman is in need of an intervention to prevent preterm birth. With incidence of preterm birth estimated at only 10%, screening may be a useful way to decipher where the high-risk cases are to aid prioritisation of resources.
References
Callaghan, William M., et al. “The contribution of preterm birth to infant mortality rates in the United States.” Pediatrics 118.4 (2006): 1566-1573.
Goldenberg, R.L., Culhane, J.F., Iams, J.D. and Romero, R., 2008. Epidemiology and causes of preterm birth. The lancet, 371(9606), pp.75-84.
Sandall, J., Soltani, H., Gates, S., Shennan, A. and Devane, D., 2016. Midwife‐led continuity models versus other models of care for childbearing women. Cochrane database of systematic reviews, (4).