Pharmacological and non-pharmacological interventions for orthodontic pain management
Posted on 2nd March 2018 by Izabel de Oliveira
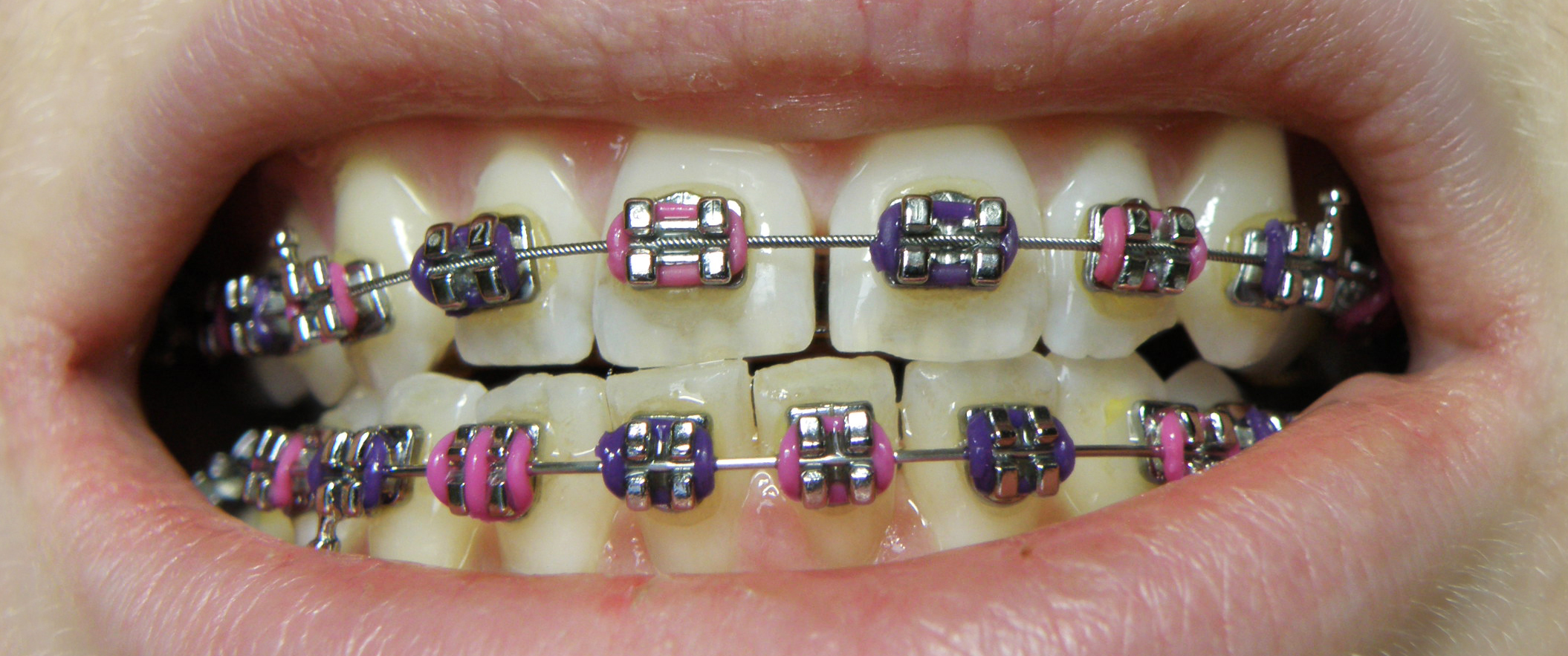
Orthodontic pain
Orthodontics is the area of Dentistry dedicated to the growth, development and relationship between dentition, jaws and face. It also involves corrective treatment of teeth and jaws when they are irregular in alignment, morphology or function. Usually, orthodontic treatment is performed to improve the function and appearance of teeth. This can involve tooth movement by applying forces through fixed, removable or functional appliances [1].
Pain is a recurrent undesirable side effect in orthodontic treatment. It is a complex phenomenon influenced by factors such as age, sex, individual pain threshold and amount of applied force. To achieve orthodontic movement, forces are applied in the dentoalveolar complex, resulting in inflammation or ischemia in the periodontal ligament with subsequent release of histamine, bradykinin, prostaglandins, substance P and serotonin. These mediators stimulate local nerve endings and send pain signals to the brain [2].
Pain experience is reported by 91% to 94% of patients undergoing orthodontic treatment.[3] Perceived as discomfort, dull pain and hypersensitivity in affected teeth, it tends to reach the peak after 24 hours, with decline after the third day of use of the appliance. Pain is a major concern for professionals and patients, and may discourage them seeking, or maintaining orthodontic treatment [4].
Management of orthodontic pain
Several strategies have been applied to relieve pain resulting from orthodontic treatment.[2] For patients experiencing greater pain, the orthodontist may recommend pharmacological or non-pharmacological methods, considering the limit of sensitivity to pain or emotional condition reported [5].
Non-steroidal anti-inflammatory drugs (NSAIDs) are the most frequently used method for pain relief. NSAIDs block the formation of arachidonic acid in the prostaglandin production cycle, which would lead to pain. Other methods include low intensity laser therapy, acupuncture, transcutaneous electrical nerve stimulation, periodontal ligament vibratory stimulation, viscoelastic bite wafers and even chewing gums. These methods can relieve compression of the periodontal ligament and restore normal vascular and lymphatic circulation in order to eliminate oedema and inflammation and reduce pain [2].
Pharmacological methods for orthodontic pain management
Non-steroidal anti-inflammatory drugs are the most popular method of pain control used during orthodontic treatment [1]. There is currently no universal recommendation on the use of analgesics,[6] however, NSAIDs are readily available, low cost, easily administered and generally harmless (in terms of lack of side effects) [1].
Ibuprofen and acetylsalicylic acid can effectively relieve orthodontic pain [1]. The analgesic action is explained by the ability to inhibit the synthesis of prostaglandins at the site of tissue injury by inhibiting the COX-1 and COX-2 cyclooxygenase enzymes [6]. They are usually administered within two hours after the orthodontic visit and during the recommended time interval in order to establish pain control. However, the use of NSAIDs is still controversial because of the potential influence on tooth movement. Prostaglandins are important mediators of bone resorption, and it has been suggested that reduced activity through NSAIDs may affect orthodontic movement even at an insignificant clinical level [1].
Paracetamol (acetaminophen) has a mechanism of action similar to that of NSAIDs, it inhibits COX with a predominant effect on COX-2. However, unlike NSAIDs, it acts on a level of the central nervous system that serves the cell membrane. As a result, inhibition of prostaglandins is minimal and use has no effect on tooth movement.[1]
Although they are reported as the most popular method for orthodontic pain control, analgesic drugs are used by only 16% to 27% of patients during the first and second days after orthodontic arch insertion [3].
Non-pharmacological methods for orthodontic pain management
Several drugs are effective in controlling pain during orthodontic treatment. However, drugs can have negative effects on tooth movement and some patients may be allergic or unwilling to use them. In order to find alternatives for pain relief, other approaches have been investigated, such as low intensity laser therapy (LLLT) [7].
The action of LLLT in reducing pain during orthodontic movement and the placement of elastic separators has been evaluated [5]. The low-intensity aluminium-gallium-indium-phosphate laser (635 nm, 6mW, 10mJ) showed efficacy when applied every 12 hours for 7 days for 30 seconds after placement of elastic separators.[8] Application of the laser diode gallium-aluminium-arsenic (810 nm, 100 mW, 2 J/cm2) for 15 seconds at each point (mesial and distal interdental papilla and near the root apex) immediately after the placement of elastic separators was effective [5]. The gallium-aluminium-arsenic diode laser (940 nm, 100 mW, 7.5 J/cm2) applied immediately after the insertion of nickel-titanium closed-coil springs for bilateral canine retraction, and with weekly intervals in the subsequent two weeks, was also able to reduce pain, and accelerate orthodontic movement.[9] Standardization of the type and use of LLLT still needs to be better established. The clinical results and the effectiveness of LLLT in reducing orthodontic pain are directly related to laser type, wavelength, energy density (J/cm2), application time per point and frequency [5].
The pulsed electromagnetic field is a non-invasive technique that has been useful as adjuvant therapy in the treatment of post-operative pain and oedema, generating small explosions of current electrical energy in injured tissues without producing heat or affecting the main biological functions. It demonstrated a significant ability to relieve orthodontic pain at 24, 48 and 72 hours after the initial orthodontic arch insertion in female subjects, applied immediately after the insertion, generating an electromagnetic field of 27.12 MHz, with power peak of 80 dbm, pulse rate of 2400 pulses per second and duration of 420 milliseconds. In this way, it can be an effective alternative to reduce the pain caused by the initial orthodontic movement [3].
There is evidence that vibratory stimulation reduces pain from teeth or surrounding tissues. Vibration can help relieve compression of the periodontal ligament, promoting normal circulation and preventing the proliferation of inflammatory by-products. Another possibility is the “gate control” theory, which suggests that pain can be reduced by the simultaneous activation of nerve fibres that lead to non-noxious stimuli. Mild micropulses (0.25 N at 30 Hz) applied daily for 20 minutes could significantly reduce the perception of pain in patients undergoing orthodontic treatment, although further studies on the technique are still needed [2].
Conclusions
- Analgesics are still the main modality of treatment to reduce orthodontic pain. However, pharmacological actions, as well as side effects, should be identified before adopting the drugs in clinical practice.
- Further studies are needed to determine effective protocols for the use of non-pharmacological methods for orthodontic pain control in clinical settings.