NHS Health Checks: what’s the evidence?
Posted on 24th July 2013 by David Carroll
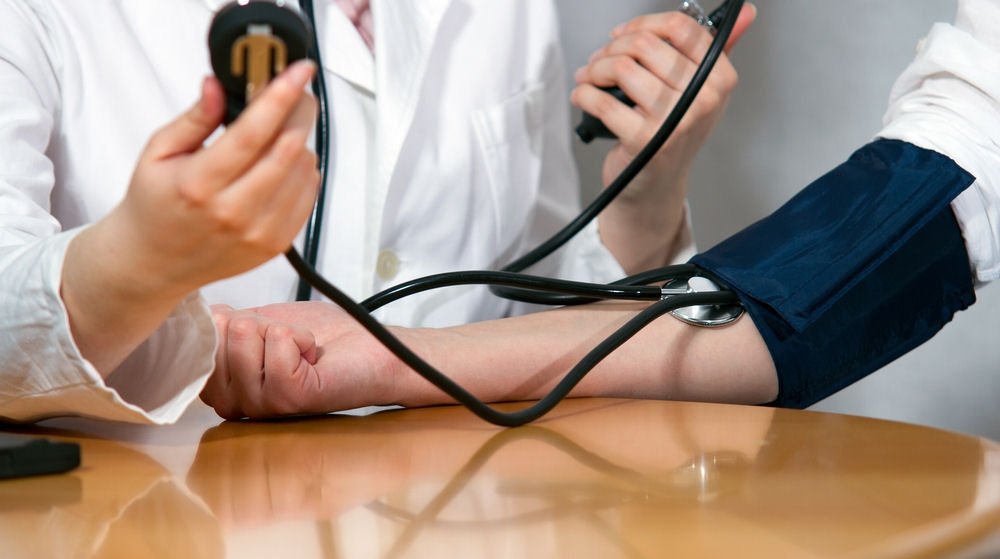
Recently the UK Government’s Secretary of State for Health, Jeremy Hunt stated “Hundreds of lives could be saved in England with better provision and take-up of free health checks“. You’d expect this to have lots of evidence to back it up. Is there any evidence to back up this claim? Let’s find out, shall we?
The NHS Health Check is for adults in England between the ages of 40 and 74. This health check involves asking questions about your age, ethnicity, smoking status, family history, physical activity and alcohol use in a check of your “personal history”. In addition to this there will be a:
- Cholesterol test.
- Blood pressure test.
- Body mass index (BMI).
- Diabetes risk assessment.
The natural assumption of people is that catching disease earlier is better. Right? Easy peasy? Sorted. Health checks will cure everything, it’s simple, it’s attractive, and it’s easy. Unfortunately though, I think you’ll find it’s more complicated than that. Screening is complex and difficult, the thing is that we’re not cars, we’re humans.
I taught some epidemiology to my fellow students earlier in this year, see some other stuff from that here. When I did this, I gave an example of a scenario of a screening test that is 90% accurate. Which is a pretty good test, right? But when you apply a really good test to a population with a low prevalence of disease, you get lots of false positives and false negatives (this also applies to David Cameron’s plans to filter the Internet too). While my imaginary disease had a really low prevalence to prove a point, this lesson is useful in the context of screening, there’s no such thing as a perfect screening test. Even the best screening tests results in false positives and false negatives. Screening tests can be useful but they can have side effects and are associated with over diagnosis, unless you have a perfect test, you will have over diagnosis. So screening is a delicate balance of benefit over harm.
A recent systematic review and meta-analysis conducted by the Cochrane Collaboration (1) (available here and here) analysed 14 trials that looked at a variety of “health-check” interventions. They found that there is no evidence to support health checks as a means of reducing population morbidity and mortality, there was no reduction for deaths from cardiovascular or cancer causes.
The results of this were that there was no change in total mortality, 9 trials gave a risk ratio of 0.99 for overall death. The eight trials that provided data on cardiovascular mortality found that screening had no effect with a risk ratio 1.03 (0.91 to 1.17), and the eight that gave data on cancer mortality gave a risk ratio of 1.01 (0.92 to 1.12), again the screening had no effect. Subgroup and sensitivity-analyses did not change these findings. Their analysis found that health checks led to a 20% increase in the total number of new diagnoses per participant over six years. Two out of four trials reported an increased use of blood pressure drugs. Two out of four trials found small beneficial effects on self-reported health, however the authors thought this could have been due to bias.
A randomised trial of screening (2) for type 2 diabetes using random capillary blood glucose and glycated haemoglobin found no significant reduction in deaths from any causes, heart disease or diabetes over 10 years. For other interventions included in this health check, like those for reducing cardiovascular risk have evidence that they work. However it is not assured that these perform as well in the context of population-based health checks.
General practitioners in the UK have to meet Quality and Outcomes Framework (QOF) targets for things like blood pressure control. If GPs fail to hit their QOF targets, not only will they lose money but also their NHS choices score will go down. These health checks should make it easier for GPs to meet their QOF targets, thus incentivising use. Public Health England also stated in the news article above that they will soon launch a website where it will be possible to show how many health check offers are being made by each local authority. This public interface will no doubt give GPs a further incentive to do health checks, as we all live in constant fear of the Daily Telegraph or the Daily Mail (well, most newspapers) looking at the figures.
So, back to the government’s “evidence”. The reference for the 650 deaths, 1,600 heart attacks and 4,000 cases of diabetes a year that will be prevented doesn’t exist. The link is broken so I can’t read it; I can’t make up my own mind about the evidence. From Twitter, I’ve been told it’s a modelled figure of 650, this type of predictive modelling is typically used when it is either impossible or impractical to do an experiment (like a trial) and directly measure outcomes. Direct measurement of outcomes under controlled conditions (see Scientific Method) will always be more reliable than modelled estimates of outcomes. I’m a relative novice in the world of evidence-based medicine and I’m sure modelling has its uses but I’m sure in this situation, using the direct method of outcomes under controlled outcomes (which is very easy to do) would be much better. Do they have such outcome data to back up their assertions? Let’s move on.
In a document produced by Public Health England, NICE and the Local Government Association called “NHS Health Check: Our Approach to the Evidence“, point 15 of this document states clearly “the NHS Health Check programme is being implemented in the absence of direct randomised controlled trial evidence to guide it”.
From this evidence…wait…what? How could you possibly…you’ve got to be kidd…there is no way…I can’t…oh my g… did they actually just say that? They did…they actually just said that. They just admitted that they have no evidence to support their decision.
I find it amazing that the Government and Public Health England, is spending public money on an intervention, which has no evidence base and there is evidence that suggests it doesn’t work. If they just didn’t know that there was no evidence to suggest it works that would “probably” make it more acceptable but the fact that they know that this has no evidence of benefit but they still continue to spend public money on is unacceptable. In the document, they speak about “how the authorities do not have time do wait for trial results”. This in itself is dangerous.
The history of medicine is littered with instances in which people have done things in the absence of evidence. There’s Dr Spock who advocated that infants should not be placed on their back when sleeping. This advice was extremely influential on health-care providers, with nearly unanimous support through to the 1990s until it was found that placing children on their abdomen was associated with a significantly increased risk of Sudden Infant Death Syndrome. There’s also corticosteroids, these drugs were used in the treatment of head injury. Until the CRASH trial, the evidence was lacking. The only evidence was small trials that varied in their suggestion of benefit or harm. When the CRASH trial (3, £) and a subsequent Cochrane Review were completed (4), we found that steroids didn’t have benefits for people with head injuries but they caused harm.
They government speaks about the need to tackle health inequalities and about how these health checks will reduce inequality. The introduction of health checks will probably do more to increase inequality. The population that attends these health checks will be largely self selecting, and participants tend to have better risk profiles (5) higher socio-economic status (6) and lower morbidity (7, £) and mortality (8, £). In fact, Evidence from a systematic review (9) showed that “routine health check-ups appear to be taken up inequitably, with gender, age, socio-demographic status and ethnicity all associated with differential service use. Furthermore, non-attenders appeared to have greater clinical need or risk factors suggesting that differential uptake may lead to sub-optimal health gain and contribute to inequalities via the “inverse care law“. What that means in English is better off; healthier people will attend health checks and inequalities will increase.
Ok, let’s go back to the modelled estimate of 650 lives that will be saved. It has been estimated 102,000 that people died in 2009 from smoking-related diseases including cancers (10). In 2011 there were 8,748 alcohol-related deaths in the UK (11). Despite this, the UK Government have recently made massive policy U-turns and dropped plans to introduce plain packaging for cigarettes and minimum alcohol pricing. Both of these are based on good evidence and the decisions to drop them have come under fire as Conservative Party’s chief election strategist, Lynton Crosby, advises Philip Morris, one of the world’s biggest tobacco companies.
I can’t understand why Public Health England are implementing a policy which doesn’t just have no evidence base but the decision makers know there is no evidence base. They appear to be doing this because doing something looks impressive. The public doesn’t care if it works as long as they’re doing something (the same with the Internet filtering stuff).
The history of routine health checks has been one of failure, but generations of people allow themselves to believe it works. The government should learn that health policy (a tricky beast to tame) should be based on good evidence of well-being, rather than on well-meant good intentions. And if the current best evidence doesn’t apply to the UK then they should explain why they don’t need evidence to implement health checks (apart from the reasons they’ve given already) or commission good quality evidence to answer this uncertainty.
References:
(1) Krogsbøll LT, Jørgensen KJ, Grønhøj Larsen C, Gøtzsche PC. General health checks in adults for reducing morbidity and mortality from disease. Cochrane Database of Systematic Reviews 2012, Issue 10. Art. No.: CD009009. DOI: 10.1002/14651858.CD009009.pub2.
(2) Simmons RK, Echouffo-Tcheugui JB, Sharp SJ et al.Screening for type 2 diabetes and population mortality over 10 years (ADDITION-Cambridge): a cluster-randomised controlled trial. Lancet 2012: Volume 380, Issue 9855
(3) CRASH trial collaborators. Final results of MRC CRASH, a randomised placebo-controlled trial of intravenous corticosteroid in adults with head injury—outcomes at 6 months. Lancet 2005: Volume 365, Issue 9475, Pages 1957 – 1959
(4) Alderson P, Roberts I. Corticosteroids for acute traumatic brain injury. Cochrane Database of Systematic Reviews 2005, Issue 1. Art. No.: CD000196. DOI: 10.1002/14651858.CD000196.pub2.
(5)Waller D, Agass M, Mant D, Coulter A, Fuller A, Jones L. Health checks in general practice: another example of inverse care? BMJ 1990;300:1115–8.
(6)Pill R, French J, Harding K, Stott N. Invitation to attend a health check in a general practice setting: comparison of attenders and non-attenders. J R Coll Gen Pract 1988;38:53–6.
(7)Jørgensen T, Borch-Johnsen K, Thomsen TF, Ibsen H, Glümer C, Pisinger C. A randomized non-pharmacological intervention study for prevention of ischaemic heart disease: baseline results Inter99. Eur J Cardiovasc Prev Rehabil 2003;10:377–86.
(8)Wilhelmsen L, Berglund G, Elmfeldt D, Tibblin G, Wedel H, Pennert K, et al. The multifactor primary prevention trial in Göteborg, Sweden. Eur Heart J 1986;7:279–88.
(9)Dryden et al. What do we know about who does and does not attend general health checks? Findings from a narrative scoping review. BMC Public Health 2012, 12 :723
(10)Mortality from smoking in developed countries 1950-2005 (or later). Peto R, Lopez A, Boreham J, et al. [Internet] 2012 [cited July 24 2013]. Available at: http://www.ctsu.ox.ac.uk/~tobacco/index.htm
(11) Alcohol-related deaths in the United Kingdom. [Internet] Office for National Statistics. 2011 [cited July 24 2013] Available at: http://www.ons.gov.uk/ons/rel/subnational-health4/alcohol-related-deaths-in-the-united-kingdom/2011/alcohol-related-deaths-in-the-uk–2011.html



No Comments on NHS Health Checks: what’s the evidence?