Delayed cord clamping revisited
Posted on 16th July 2013 by Alice Buchan
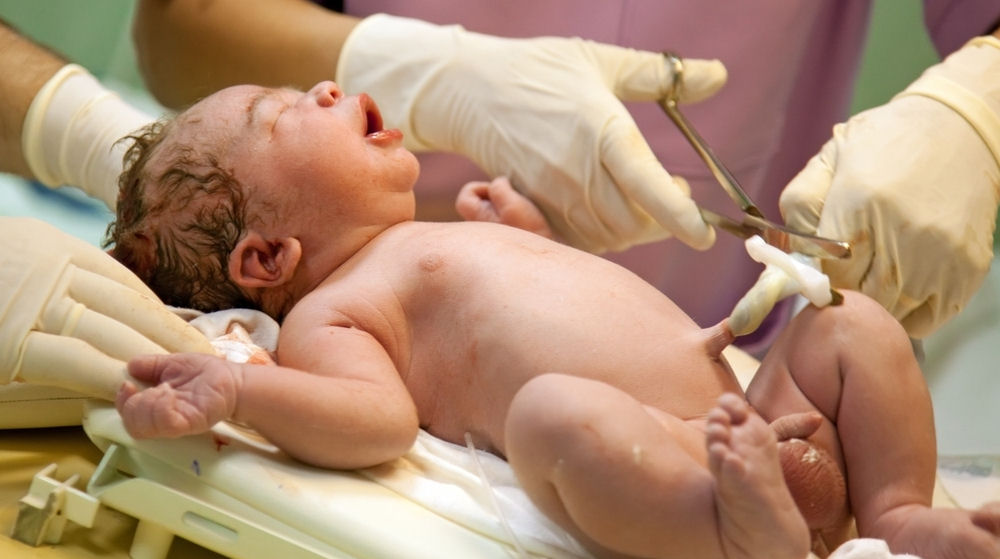
I blogged about the evidence surrounding early and late clamping of the umbilical cord after childbirth some time ago, and on Thursday, an updated Cochrane review on the subject came out, prompting me to (briefly) revisit my original blog. Since the original blog was in part based on the previous 2008 version of this new review, I shall start by considering what has changed between the two reviews.
What’s new?
Firstly, the newer version [1] includes 15 trials and nearly 4,000 mother and infant pairs, compared to the 2008 version [2], which includes 11 trials and nearly 3,000 mother and infant pairs. There are also some different outcomes, which are grouped differently. In the 2008 review they are first sorted into maternal and newborn outcomes, whereas in the most recent version they are arranged as primary and then maternal and neonatal secondary outcomes. I personally find this arrangement of the most serious outcomes (severe postpartum haemorrhage, maternal death, and neonatal death) a good way of balancing the fact that the best outcome may be a balance of what is best for the mother and best for the newborn. There are also 2 new secondary outcomes in the 2013 review – birth weight and symptoms of infection.
The recommendation from the Cochrane review remains similar – delayed cord clamping may increase the iron stores in the newborn, and the inclusion of 4 new trials in the 2013 version strengthens their conclusion as the body of evidence supporting it is now substantially greater. Both versions of the review add the caveat that this should be considered where phototherapy for neonatal jaundice is available, as rates of jaundice requiring phototherapy increased in the delayed clamping group.
Implications
As mentioned in my earlier blog, the National Institute for Health and Care Excellence (NICE) guidance currently recommends early clamping of the umbilical cord, as part of active management of the third stage of labour [3]. This group of interventions has reduced maternal mortality and postpartum haemorrhage but the evidence now suggests that cord clamping may not prevent haemorrhage. The evidence still supports the use of a uterotonic drug [4] (reviews of other uterotonics are also out there) compared to no drug; there is a protocol for a Cochrane review of controlled cord traction at [5], although several studies have recently come out finding little orno increase in risk of haemorrhage without its use, but with the use of a uterotonic [6] [7].
As a medical student, the aphorism ‘half of what you learn at medical school is wrong’ is oft-quoted. I don’t doubt that there will be (evidence-based) paradigm shifts in many fields, including obstetrics over my career, and probably before I qualify in 3 years time!
For more on delayed clamping of the umbilical cord, take a look at the Evidently Cochrane blog on the same review here.
Links:
[1] McDonald SJ, Middleton P, Dowswell T, Morris PS. Effect of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes. Cochrane Database Syst Rev. 2013;CD004074 Available online: http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD004074.pub3/full
[2] McDonald SJ, Middleton P. Effect of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes. Cochrane Database Syst Rev. 2008;CD004074.pub2 Available online: http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD004074.pub2/full
[3]National Collaborating Centre for Women’s and Children’s Health. Intrapartum Care: care of healthy women and their babies during childbirth. 2007. [Cited 15 July 2013] Available online: http://www.nice.org.uk/nicemedia/pdf/CG55FullGuideline.pdf
[4] Liabsuetrakul T, Choobun T, Peeyananjarassri K, Islam QM. Prophylactic use of ergot alkaloids in the third stage of labour. Cochrane Database Syst Rev. 2009;CD005456.pub2 Available online:
http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD005456.pub2/abstract
[5] Mshweshwe NT, Hofmeyr GJ, Gülmezoglu AM. Controlled cord traction for the third stage of labour. Cochrane Database Syst Rev. 2009;CD008020 Available online: http://onlinelibrary.wiley.com/doi/10.1002/14651858.CD008020/abstract
[6] Gülmezoglu AM, Lumbiganon P, Landoulsi S, Widmer M, Abdel-Aleem H, Festin M, Carroli G, Qureshi Z, Souza JP, Bergel E, Piaggio G, Goudar SS, Yeh J, Armbruster D, Singata M, Pelaez-Crisologo C, Althabe F, Sekweyama P, Hofmeyr J, Stanton ME, Derman R, Elbourne D. Active management of the third stage of labour with and without controlled cord traction: a randomised, controlled, non-inferiority trial. Lancet. 2012;379:1721-7
[7] Deneux-Tharaux C, Sentilhes L, Maillard F, Closset E, Vardon D, Lepercq J, Goffinet F. Effect of routine controlled cord traction as part of the active management of the third stage of labour on postpartum haemorrhage: multicentre randomised controlled trial (TRACOR). BMJ 2013;346:f1541


No Comments on Delayed cord clamping revisited
Since your blog the new NICE intrapartum care guideline is out recommending delayed cord clamping for at least one minute and up to five minutes. This recognises that the timing of cord clamping has no influence on the risk of PPH but a big influence on the health of the baby. If you read the Macdonald Cochrane review fully you will see that most of the “need for phototherapy” comes from her own unpublished study. This study is available at the Univeristy of Liverpool and shows a very large number (>30%)of protocol violations in the delayed cord clamping arm. Therefore it is quite possible that early cord clamping leads to a need for phototherapy. This indeed was the finding of the latest Andersson study where there were slightly FEWER babies in the delayed cord clamping arm who needed phototherapy. A proper understanding however of the circualtion transition at birth soon makes it obvious that early cord clamping is a significant intervention for the baby and a recent paper in ADC concluded that clamping before the onset of established respiration (ie early) can lead to severe hypoxic/ischamic cerebral circulation. Hooper SB, et al. Arch Dis Child Fetal Neonatal Ed 2014;0:F1–F6.
4th January 2015 at 4:40 pmWicked blog Alice, do you think the way the outcomes were group affected the analysis?
I would read it myself but I’m in America and I CAN’T ACCESS IT.
17th July 2013 at 4:39 amThanks David! As far as I’m aware, all the outcomes (maternal /newborn, primary/secondary) were assessed individually in both the 2008 and the 2013 versions – there doesn’t appear to be a statistical synthesis into one outcome (probably not that useful and almost impossible given the number and types of outcomes and that they are for 2 patients) so I would say that the structure made it clearer which outcomes were priorities when the authors were considering their recommendation, but didn’t change the statistical analysis itself. Good point though – might have to ask about that one!
17th July 2013 at 8:16 am