Delayed cord clamping: simple but effective?
Posted on 29th April 2013 by Alice Buchan
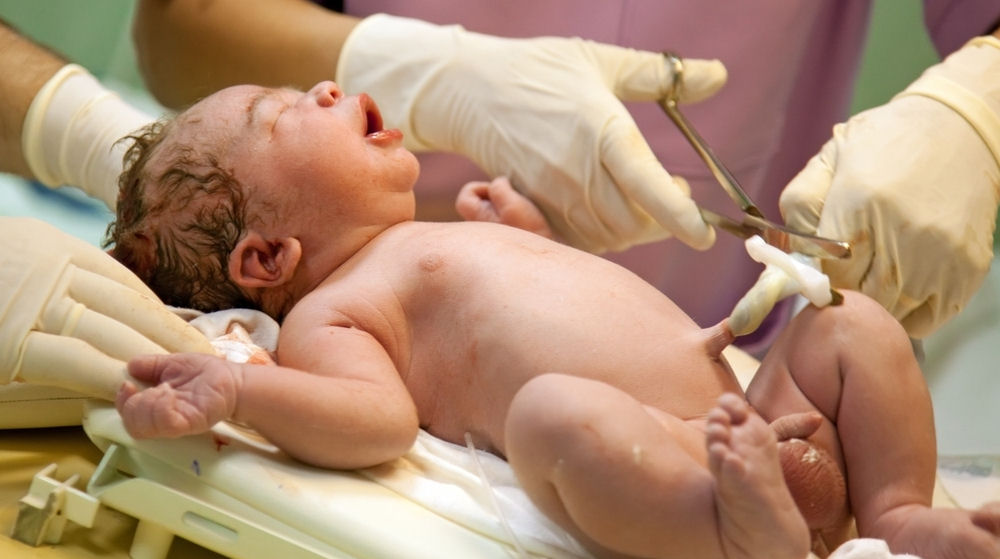
Care of babies immediately after birth may be set to change in the UK. NICE (The National Institute for Health and Care Excellence) have reportedly decided to review their guidelines on care in normal births [1], specifically the management of the third stage of labour, in which the umbilical cord is cut and the placenta is delivered. The current guidance, first written in 2007 [2], and earmarked for review in 2011[3], suggests that ‘active management’ of the third stage is preferred, although if the woman chooses ‘physiological management’, her decision should be supported.
As defined by NICE in their guidelines, active management consists of three major interventions: clamping the umbilical cord early, routine use of an uterotonic (contraction-inducing) drug, and controlled cord traction. These interventions aim to reduce the risk of postpartum haemorrhage, and the volume of a haemorrhage should one occur. By contrast, physiological management consists of delayed cord clamping, and a natural delivery of the placenta without uterotonic drugs or cord traction. The guidelines are likely to change in favour of promoting delayed cord clamping, although other aspects of active management may remain.
There are two major reasons for considering a change – firstly, that clamping the umbilical cord immediately after birth may not actually reduce risk of postpartum haemorrhage, and secondly, that delayed cord clamping may reduce the risk of iron-deficiency anaemia in the infant, even several months after birth. Delayed cord clamping allows a substantial volume of blood to flow from the placenta back into the baby, resulting in a greater blood volume. A 2008 Cochrane review of the trials of early versus delayed cord clamping in infants born at term found no significant differences in the rates of postpartum haemorrhage or severe postpartum haemorrhage (>1000mL blood loss) between the early and late cord clamping groups [4]. There was also no statistically significant increase in the length of the third stage of labour. The neonates included in this review whose umbilical cords had been clamped later had significantly greater haemoglobin levels 24-48 hours after birth, as well as a significantly greater incidence of neonatal jaundice requiring phototherapy. They also had significantly increased ferritin levels compared to the early clamping group.
 Last year, a Cochrane review looked at the effects of delayed cord clamping in pre-term infants (defined as birth earlier that 37 weeks gestation) [5]. There has been concern that delayed clamping in babies born prematurely may delay important medical interventions, leading to worse outcomes. This systematic review found that delayed clamping actually led to improvements in terms of blood pressure, lower risk of needing a blood transfusion, and also of two severe complications of pre-term birth: intraventricular haemorrhage and necrotizing enterocolitis.
Last year, a Cochrane review looked at the effects of delayed cord clamping in pre-term infants (defined as birth earlier that 37 weeks gestation) [5]. There has been concern that delayed clamping in babies born prematurely may delay important medical interventions, leading to worse outcomes. This systematic review found that delayed clamping actually led to improvements in terms of blood pressure, lower risk of needing a blood transfusion, and also of two severe complications of pre-term birth: intraventricular haemorrhage and necrotizing enterocolitis.
A 2011 study in the BMJ looked at the long-term outcomes of delayed cord clamping [6]. They used sealed-envelope randomisation, and followed up the infants after 4 months. Those in the delayed cord clamping group had substantially higher ferritin levels at 4 months; ferritin levels are considered a good measure of overall iron status. Significantly fewer infants in the delayed clamping group were considered iron-deficient.
The evidence would seem to be stacked up in favour of delayed cord clamping as it improves iron status in infancy, and does not increase risk of complications to the mother. Several hospitals are using delayed clamping as standard, practicing based on the evidence, rather than the guidelines. The guidelines for this aspect of care during childbirth may soon be evidence-based.
References:
[1] Denis Campbell. Cutting cord too early puts babies at risk, NHS warned. The Guardian. 25 April 2013. [Cited 28 April 2013] Available online: http://www.guardian.co.uk/society/2013/apr/25/cutting-cord-babies-risk-nhs
[2] National Collaborating Centre for Women’s and Children’s Health. Intrapartum Care: care of healthy women and their babies during childbirth. 2007. [Cited 28 April 2013] Available online: http://www.nice.org.uk/nicemedia/pdf/CG55FullGuideline.pdf
[3] NICE. Review of Clinical Guideline (CG55) – Intrapartum Care. February 2011. [Cited 28 April 2013] Available online: https://www.nice.org.uk/guidance/cg55/documents/cg55-intrapartum-care-review-decision2
[4] McDonald S, Middleton P. Effect of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes. Cochrane Database of Systematic Reviews. 2008. CD004074. [Cited 28 April 2013]
[5] Rabe H, Diaz-Rossello JL, Duley L, Dowswell T. Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes. Cochrane Database of Systematic Reviews. 2012. CD003248 [Cited 28 April 2013]
[6] Andersson O, Hellström-Westas L, Andersson D, Domellöf M. Effect of delayed versus early umbilical cord clamping on neonatal outcomes and iron status at 4 months: a randomised controlled trial. BMJ 2011;343:d7157 [Cited 28 April 2013]




No Comments on Delayed cord clamping: simple but effective?
Corrected link: http://ow.ly/mR77u
11th July 2013 at 11:15 am