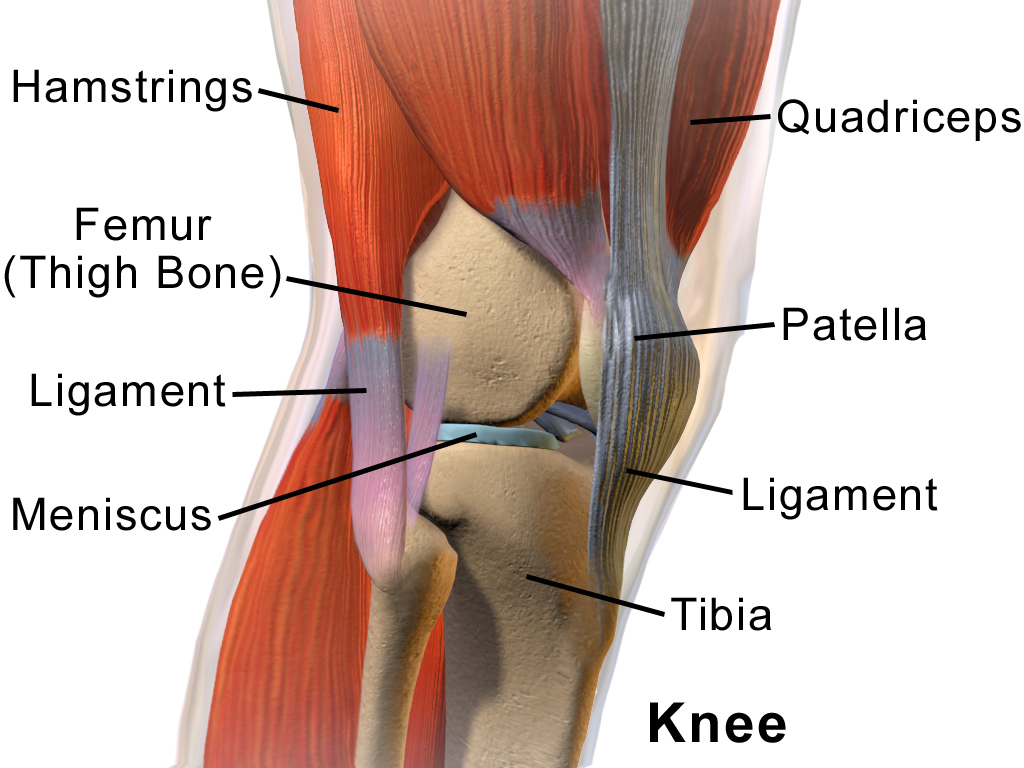
Effectiveness of individually tailored pre-arthroplasty rehabilitation
Posted on 18th January 2016 by Elizabeth

Introduction
During my first placement with an elective orthopedic team, I was surprised by the fact that over 80% of patients (NHS FIFE) were discharged within 3 days after their major elective arthroplasty. Through my patients’ feedback, I suspected that this was due to having appropriate, good quality pre-operative information on what to expect from all of the multi disciplinary professionals involved in their care.
Arthroplasty is a surgical procedure, where the function and integrity of the joint which has been affected by degenerative joint conditions is restored through resurfacing the bone or replacing it with an artificial prosthesis.
According to the Scottish Arthroplasty Project ‘Biennial Report 2014’, the number of arthroplasty operations has increased over the past 7 years (7609 hip and 7169 knee arthroplasty operations were performed in 2013), costing the NHS on average £7000 per patient (SCOTTISH ARTHROPLASTY PROJECT 2014). This cost increases according to the length of inpatient stay which can vary according to complications or other comorbidities. Even though I was satisfied with the departmental audit data on the benefits of following an accelerated recovery protocol, I was interested in finding more evidence from different research. This led me to this article:
CROWE, J. and HENDERSON, J., 2003. ‘Pre-arthroplasty rehabilitation is effective in reducing hospital stay’. Canadian journal of occupational therapy. April, Vol.70, no.2, pp.88-96. [viewed 09 January 2016]. Available from: http://www.ncbi.nlm.nih.gov/pubmed/12704972
What did they look at?
The purpose of this study was to look at the effectiveness of patient centred rehabilitation of patients, who were undergoing lower extremity arthroplasty and the effects of that on their functional capacity and on cost.
133 subjects who were scheduled for an elective arthroplasty (hip or knee) with complex needs (limited social support, comorbidities such as hypertension, transient ischemic attacks and other comorbidities), with a high score on Oxford Hip or Knee Questionnaire (with higher scores indicating greater problem severity) and a low functional performance score were placed in this randomized controlled trial.
After randomly assigning 68 clients to a ‘control subject group’ and 65 clients to a ‘rehabilitation subject group’ the control subject group received one standard pre operative clinic visit. This included assessments from a physician and nurse, required tests and a brief education on preoperative medications, bowel preparation and some information on post operative phase and temporary functional limitations. The ‘rehabilitation subject group’ received a one to one pre-operative assessment from a nurse, occupational therapist and a physiotherapist who looked at that client’s specific needs and goals. They also received an educational package which included a 50 minute video, booklets & equipment (which focused on either hip or knee arthroplasty), featuring detailed information on what to expect at each stage and what their responsibilities were, information on how to use equipment (such as walking aids, long handed shoehorns, a reacher, tights or sock aids) and also interviews with previous clients.
These clients were also provided with specific advice from an occupational therapist and physiotherapist and information on strengthening, range of motion (ROM) exercises, energy conservation, work simplification, wound care, pain control, anticoagulants (medication to help reduce blood clots), social care input and home alterations. All subjects received the same quality and quantity of post operative care such as analgesia and anaesthesia.
What was measured?
Pre and post operative outcome measures such as Hip or Knee Oxford Questionnaires, self reporting scales measuring pain and disability, functional performance, cognitive status and certain components of the Spielberger State Anxiety Inventory (STAI) were also completed. The most important outcome measure was the number of days to achieve discharge criteria. Such as; to be able to transfer from bed, mobilize independently with or without aids (30 meters) with minimal assistance, negotiate a number of stairs, 50° active range of movement (ROM) for knee arthroplasty patients and 40° active ROM for hip arthroplasty patients. They were also required to have adapted equipment such as gait aids, raised toilet seats etc. All outcome measures had a high internal consistency, and good test-retest reliability.
Results
Average number of days for discharge was shorter for the rehabilitation subject group than the control group (6.55 days vs. 10.5 days respectively), with statistical significance (p value) of 0.032. Since the rehabilitation group was well prepared with plans in place before their surgery, they had more time to spend on their physical rehabilitation with the professionals. Control subjects were more anxious at preoperative visit, scoring 45.7 on the STAI versus rehabilitation subjects scoring 40.0. One limitation of the study though is that, due to the patient centred nature of the interventions for the rehabilitation group, the input they received is not easily quantified. Other limitations such as relying on self report and not having an appropriate physical performance test apart from function performance were also evident. Nonetheless, based on these results, the authors concluded that pre rehabilitation programs before arthroplasty are effective and cost efficient.
Take home message
Even though it’s important to look at a range of research in order to provide a safe and cost effective service, this research shows us the importance of providing patient centred care and the effect it can have on a patient. Even though it can be time consuming to provide detailed pre operative advice and costly to produce evidence based information, evidence such as this trial shows its long term cost effectiveness and positive effects on patient satisfaction.
References
CROWE, J. and HENDERSON, J., 2003.’Pre-arthroplasty rehabilitation is effective in reducing hospital stay’. Canadian journal of occupational therapy. April, Vol.70, no.2, pp.88-96. [viewed 09 January 2016]. Available from: http://www.ncbi.nlm.nih.gov/pubmed/12704972
SCOTTISH ATHROPLASTY PROJECT., 2014. Biennial report. [Online]. Scotland: NHS. [Viewed 10 January 2016]. Available from: http://www.arthro.scot.nhs.uk/docs/2014-08-12-SAP-Report.pdf?2